Shoulder Instability
What is the shoulder?
The shoulder is a complex ball-and-socket joint that allows full movement of the arm.
It offers a wide range of motion, but is vulnerable to injury.
At the shoulder, three major bones meet and create a 90-degree angle. These bones are the collarbone (clavicle), the shoulder blade (scapula) - commonly known as the shoulder blade and the humerus.
Three joints are formed from the junctions of these three bones and the sternum. These joints are the glenohumeral joint, the acromioclavicular (AC) joint and the sternoclavicular joint.
Each joint in the shoulder is surrounded by cartilage for padding, ligaments to connect the bones, muscles and tendons to attach the muscles to the bones.
What is Shoulder Instability?
Shoulder instability is a condition causing dislocation or subluxation of the shoulder joint.
A dislocation occurs when the end of the humerus, the ball portion, completely dislocates from the glenoid, the socket portion of the shoulder. A partial dislocation is referred to as a subluxation
Shoulder Instability increases the chance of further dislocation with every occurrence due to damage and stretching of tissues and ligaments.
Causes of Shoulder Instability
- Injury resulting in a partially or completely dislocated shoulder
- Degeneration
- Repetitive stress
- Generalised ligamentous laxity, commonly referred to as being double jointed
Shoulder Instability symptoms
Shoulder Instability generally causes pain and sufferers have the following symptoms:
- Some patients suffer little to no symptoms
- Repeated Shoulder dislocations
- Repeated instances of the shoulder giving out
- Pain during activates
- Pain at night and the following morning
- A sensation of the shoulder joint moving out of place
- Numbness in the arm
Diagnosis of Shoulder Instability
Dr Biggs will need to diagnose the specific nature of shoulder instability. Often, shoulder instability can be identified during a physical exam by a medical professional. By examining the joint the cause of symptoms can be pinpointed.
Diagnostic methods include:
Consultation - During this consultation Dr Biggs will:
- Take a medical history
- Perform a physical examination
- Assess the joint’s range of motion
Imaging tests - In order to clearly understand the nature of any loss of the joint space or bone spur formation imaging scans are required:
- X-rays- these pictures will show injuries to the bones that make up the shoulder joint.
- MRI - can create detailed images of both hard and soft tissues. An MRI can produce cross-sectional images of internal structures required if the diagnosis is unclear.
While not all of these approaches or tests are required to confirm the diagnosis, this diagnostic process will also allow Dr Biggs to review any possible risks or existing conditions that could interfere with the surgery or its outcome.
Shoulder Instability Treatments
Shoulder instability is often treated with nonsurgical options, however this is not always successful. If these options do not relieve the pain and instability, surgery may be needed.
Surgery is often necessary to repair torn or stretched ligaments so that they are better able to hold the shoulder in place.
Non Surgical Treatments:
- Immobilisation
- Physiotherapy
Shoulder Instability Surgery
Shoulder Stabilisation surgery may improve stability and function to the shoulder joint and prevent recurrent dislocations.
Shoulder stabilisation surgery has traditionally been performed as open surgery, with large incisions and a long recovery process.
Minimally Invasive Shoulder Surgery
Shoulder Stabilisation surgery can now be performed arthroscopically, depending on the patient’s particular situation, with much smaller incisions. Occasionally, however, arthroscopic surgery may need to be converted to open surgery to properly repair the damage to internal structures.
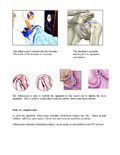
Two or three small incisions(portals) are made.
In one portal, the arthroscope is inserted to view the shoulder joint. Along with the arthroscope, a sterile solution is pumped to the joint which expands the shoulder joint, giving the surgeon a clear view and room to work.
With the images from the arthroscope as a guide, the surgeon can look for any pathology or anomaly. The large image on the television screen allows the surgeon to see the joint directly and to determine the extent of the injuries, and then perform the particular surgical procedure, if necessary.
This may involve repairing a tear in the labrum as well as tightening the capsule and ligaments.
After stabilising the shoulder, the portals (incisions) are closed by sutures.
Untreated Shoulder Instability
Shoulder Instability is not life threatening but can severely impact a patient’s quality of life and function.
It can affect anyone: elite athletes and the active individual, manual labourers and office workers.
Damage to tendons can lead to
- Short Term Impact - ongoing pain and disability.
- Long Term Impact - damage becomes permanent.
Shoulder Stabilisation Surgery Risks
As with any major surgery there are potential risks involved. The decision to proceed with the surgery is made because the advantages of surgery outweigh the potential disadvantages.
It is important that the patient is informed of these risks before the surgery takes place.
Complications can be medical (general) or specific to surgery.
Medical complications include those of the anaesthetic and your general well being. Almost any medical condition can occur so this list is not complete. Complications include:
- Allergic reactions to medications
- Blood loss requiring transfusion with its low risk of disease transmission
- Heart attacks, strokes, kidney failure, pneumonia, bladder infections.
- Complications from nerve blocks such as infection or nerve damage.
Serious medical problems can lead to ongoing health concerns, prolonged hospitalisation or rarely death.
Specific complications for surgery are rare but may include:
Infection - Infections can occur superficially at the incision or in the joint space of the shoulder, a more serious infection. Infection rates vary; if it occurs it can be treated with antibiotics but may require further surgery.
Shoulder Stiffness - Shoulder stiffness with loss of range of motion is a common complication that can be greatly minimized with strict adherence to your occupational therapy program prescribed by your surgeon.
Dislocations - Dislocations and/or subluxations with activity can occur before healing has taken place. It is very important that you follow your surgeon’s guidelines for activity restrictions.
Damage to nerves of Blood Vessels - Also rare but can lead to weakness or loss of sensation in part of the arm. Damage to blood vessels may require further surgery if bleeding is ongoing.
Damage to the joint - Joint damage to the cartilage or other structures can occur during surgery and may require another operation to repair.
Blood Clots (Deep Venous Thrombosis) - Blood Clots can form in the arm muscles and can travel to the lung (Pulmonary embolism). These can occasionally be serious and even life threatening. If the patient suffers arm pain, redness or swelling, or have shortness of breath at any stage, contact Dr Biggs
Surgery Preparation
Once Dr Biggs decides that surgery is required, preparation is necessary to achieve the best results and a quick, problem free recovery.
Preparing mentally and physically for surgery is an important step toward a successful result.
- Dr Biggs will create a treatment plan and
- patients will also need to understand the process and their role in it
Participating and completing a tailored exercise program before (ie. pre-hab) with a trained physiotherapist will achieve the best result after surgery.
Dr Biggs will also need to:
- Discuss any medications being taken with your doctor or physician to see which ones should be stopped before surgery
- Do not eat or drink anything, including water, for 6 hours before surgery
- Stop taking aspirin, warfarin, anti-inflammatory medications or drugs that increase the risk of bleeding one week before surgery to minimise bleeding
- Review blood replacement options (including banking blood) with your doctor
- Stop or cut down smoking to reduce your surgery risks and improve your recovery
Report any infections to Dr Biggs prior to surgery as the procedure cannot be performed until all infections have cleared up.
Post Shoulder Stabilization Surgery
The patient will wake up in the recovery room and then be transferred back to their hospital room.
- Pain medication will be provided to keep the patient comfortable.
- A bandage will be around the operated shoulder and the arm will be in a sling or brace.
- The sling will be worn for about 4-6 weeks to facilitate healing.
Dr Biggs will see the patient prior to discharge and explain the findings of the operation and what was done during Surgery.
- The bandage will usually be removed 48 hours post surgery and place dressings provided by your surgeon over the area.
- It is normal for the shoulder to swell after the surgery.Placing Ice-Packs on the shoulder will help to reduce swelling. Ice packs should be applied to the area for 20 min 3-4 times a day until swelling has reduced.
The patient should keep a pillow under their elbow while lying in bed.
- The patient will not be allowed to lift anything over your head or anything greater than 1 kilo for the first 6 weeks.
- 7-10 days after surgery Dr Biggs will see the patient to monitor their progress and remove the sutures.
It is recommended that the patient not drive during the first 6 weeks while wearing a sling due to safety reasons and the risk of injury to the surgical site.
The patient will be given specific instructions regarding activity and a rehabilitation program of exercise and strengthening.
Eating a healthy diet and not smoking will promote healing.
Surgery for Shoulder Instability - Patient Info Handouts
![]() Click here to download the PDF
Click here to download the PDF
Post-operative protocol following arthroscopic shoulder stabilisation